10 Hypokalemia Symptoms
Hypokalemia or low potassium in the blood refers to levels lower than 3.5 mmol/l. The normal levels of potassium range from 3.5 to 5.0 mmol/l. Mild hypokalemia does not usually cause symptoms. There are many causes of hypokalemia such as diarrhea, diabetes insipidus, dialysis, hypomagnesemia, hyperaldosteronism, side effect of medications like furosemide or steroids, and more. Hypokalemia is thought to be severe if serum potassium levels become lower than 2.5 mmol/l. It can be diagnosed using a blood test and electrocardiogram. The treatment of hypokalemia involves the replacement of potassium.
However, potassium replacement should be done with care depending on the changes seen on the electrocardiogram. Mild hypokalemia can be managed via dietary changes. Oral or intravenous potassium supplements can be provided. While intravenous potassium can be given at 20 mmol per hour, high concentrations of more than 40 mmol/l should be administered through a central line. Magnesium replacement may also be needed during potassium replacement. Hypokalemia is one of the commonest water-electrolyte imbalances and can affect as many as 20 percent of admitted patients in the hospital.

Symptom #1: Muscle Cramps
A muscle cramp occurs when there is a sudden and involuntary muscle contraction that is usually non-damaging and transient. Muscle cramps can also cause immobility and pain of the affected muscle. It usually has a sudden onset and will resolve on its own.
Cramps can affect both skeletal or smooth muscles. In skeletal muscle cramps, causes include hyponatremia, muscle fatigue, hypokalemia, or hypomagnesemia. Causes of smooth muscle cramps include gastroenteritis, menstruation, and more.

Symptom #2: Fatigue
Fatigue is a gradual onset of tiredness where it can be alleviated by rest. It can be divided into physical and mental fatigue where physical fatigue is the temporary inability to maintain peak muscle performance. Mental fatigue occurs when there is a transient inability to maintain peak cognitive performance. It can manifest in patients as somnolence or lethargy.
Being a non-specific and common symptom, it can be seen in many conditions like stress, overworking, jet lag, depression, overstimulation, boredom, inadequate sleep, hypoglycemia, mineral deficiencies, and more.

Symptom #3: Arrhythmia
An abnormal heart rhythm is known as an arrhythmia. This term represents a group of conditions where the heartbeat is irregular, too slow, or too fast. Tachycardia occurs when the heart beat is more than 100 beats per minute while bradycardia occurs when the heart rate is less than 60 beats per minute.
Types of arrhythmia include bradyarrhythmias, ventricular arrhythmias, extra beats, supraventricular tachycardia, and more. Arrhythmia occurs when there are issues with the electrical conduction in the heart or electrolyte imbalances such as hypocalcemia or hypokalemia.

Symptom #4: Constipation
Constipation occurs when the bowel movements become infrequent or hard to pass. The stool can be described to be hard and dry. Constipation is often associated with symptoms such as abdominal pain and bloating. Complications include hemorrhoids, anal fissure, or fecal impaction.
Constipation can occur in conditions such as hypothyroidism, diabetes, irritable bowel syndrome, pelvic floor issues, celiac disease, colon cancer, diverticulitis, side effect of medications, and more. Depending on the underlying cause of constipation, treatment may involve consumption of more fiber, drinking more fluids, exercise, and the use of laxatives.

Symptom #5: Muscle Weakness
Muscle weakness is also known as myasthenia. The term “myasthenia” is of Greek origin and can be translated to mean lack of muscle strength. Weakness can be divided into true or perceived weakness where true muscle weakness is caused by conditions such as muscular dystrophy and inflammatory myopathy.
Other causes include imbalances of electrolytes such as hypokalemia. Perceived muscle weakness occurs when the affected individual feels that more effort is necessary to exert a given amount of force despite having normal muscle strength.
Symptom #6: Hypertension
Hypertension is a term that describes high blood pressure. The blood pressure is a measurement of the pressure on the walls for blood vessels. It is used to measure the pressure in large arteries and expressing it in systolic and diastolic pressure.
Blood pressure can be affected by factors such as cardiac output, total peripheral resistance, and arterial stiffness. Studies have also shown that potassium levels can affect blood pressure levels. It was demonstrated that a low potassium intake increases blood pressure while a higher potassium intake lowers blood pressure.

Symptom #7: Flaccid Paralysis
Flaccid paralysis occurs when there is reduced muscle tone, weakness, and paralysis without an apparent cause (like trauma). It can be caused by injuries or diseases that impact the nerves. A severed nerve that supplies a muscle group will result in flaccid paralysis in that group of muscles where the affected part of the body appears to be limp.
Flaccid paralysis can result in fatality if it involves the muscles of respiration as it causes the patient to be unable to breathe and eventually die from suffocation. Examples of diseases that can cause flaccid paralysis include botulism, polio, lower motor neuron lesions, curare, neurotoxic venoms, nerve agents, hypokalemia, and more.
Symptom #8: Myalgia
Myalgia is a term that refers to muscle pain. Muscle pain is a common and non-specific symptom that is observed in many disorders and conditions. The commonest cause of myalgia is due to the overuse and overstretching of muscle groups. However, it can also be caused by metabolic myopathy, viral infections, chronic fatigue syndrome, side effect of medications, nutritional deficiencies, multiple sclerosis, fibromyalgia, and more.
Treatment for myalgia depends on the underlying cause but can be managed symptomatically with pain medication such as paracetamol (acetaminophen) and NSAIDs such as diclofenac sodium and ibuprofen.
Symptom #9: Respiratory Depression
Respiratory depression or hypoventilation occurs when there is inadequate ventilation required for gas exchange. It results in the increased concentration of carbon dioxide throughout the body. This is known as hypercapnia and results in respiratory acidosis.
It can be seen in conditions such as a stroke affecting the brainstem, use of medications or drugs, voluntary breath holding, chronic mountain sickness, hypokalemia, etcetera. It should be considered a medical emergency and patients should seek medical attention as soon as possible.
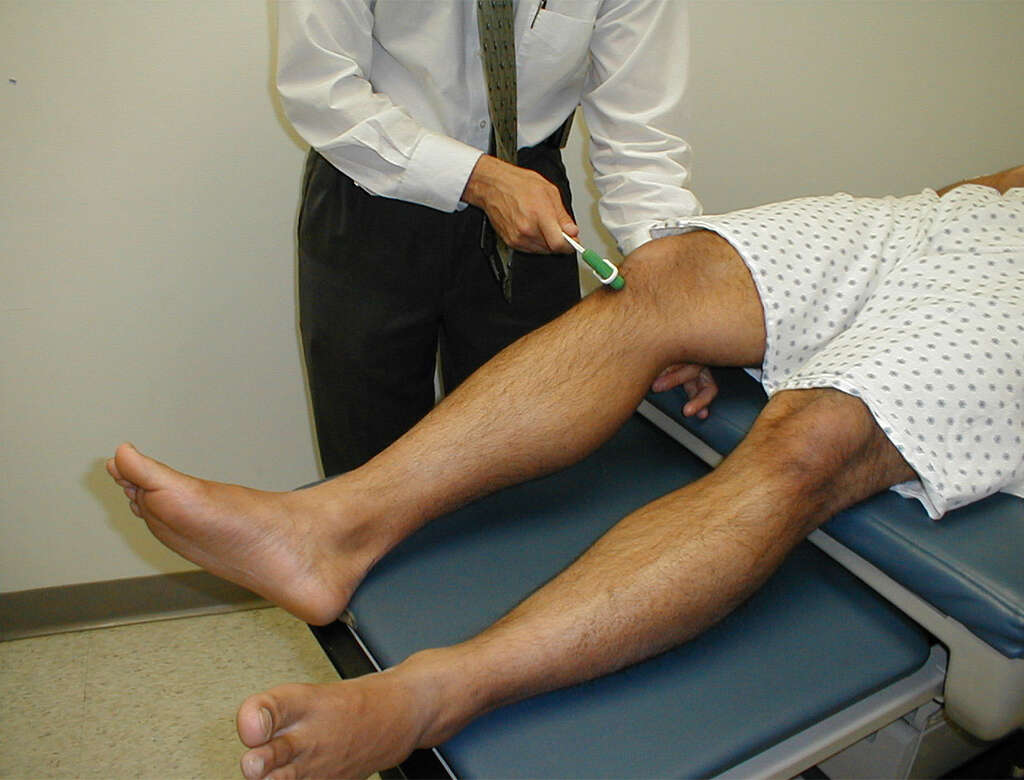
Symptom #10: Hyporeflexia
Hyporeflexia is a term describing absent or below normal reflexes. To detect and examine reflexes, a reflex hammer can be used. Hyporeflexia can be linked to a lower motor neuron deficit. It can be seen in conditions such as Guillain-Barre syndrome, electrolyte imbalance, hypothyroidism, spinal cord injury, side effect of drugs, polyneuropathy, and more.
Hyporeflexia is usually temporary and resolves once the potassium levels in the blood are corrected and back to normal.