10 Side Effects of Spinal Taps
A spinal tap or lumbar puncture is a procedure where a needle is inserted into the spinal canal for the collection of cerebrospinal fluid for diagnosis purposes. The most common reason for a spinal tap is for the diagnosis of diseases that involve the central nervous system. Examples of these diseases include meningitis, infection, medulloblastoma, and carcinomatous meningitis.
A spinal tap may also be used for therapeutic purposes in some conditions. One main contraindication of a spinal tap is increased intracranial pressure as it can result in further complications.
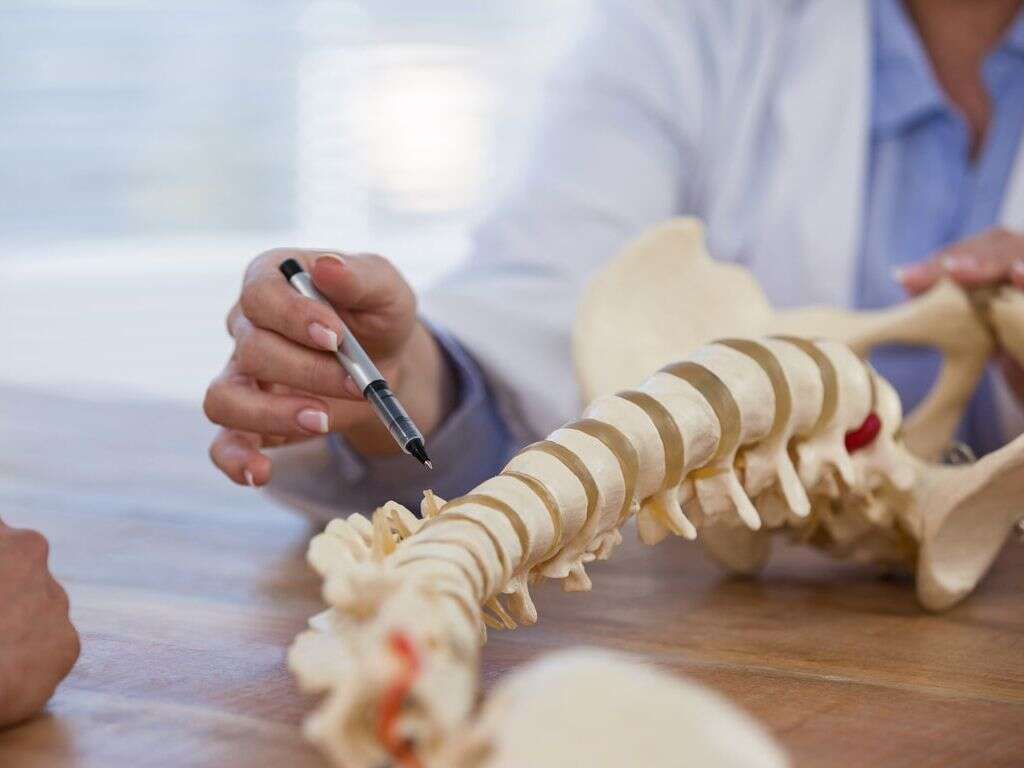
A spinal tap is usually performed under local anesthesia with a sterile technique. The patient is first placed on their side with their knees to the chest. The lower back is then prepared, palpated, and injected with local anesthesia. A hypodermic spinal needle is inserted between the third and fourth lumbar vertebrae or between the fourth and fifth lumbar vertebrae. It is pushed through the meninges, the protect layering around the spinal cord and brain, to the level of the subarachnoid space which contains the cerebral spinal fluid (CSF). A sample of CSF is then collected.
Side Effect #1: Postdural Puncture Headache
A postdural puncture headache is a common complication of a spinal tap. The headache is often described as severe, searing, and spreads “like hot metal,” involving both the back and front of the head. The headache may radiate to the shoulders and neck. Other associated symptoms include neck stiffness, hearing loss, nausea, tinnitus, vomiting, vertigo, paresthesia of the scalp, and dizziness.
It is a common side effect seen after lumbar puncture and spinal anesthesia. This is due to the leakage of cerebrospinal fluid leading to the reduced fluid levels in the spinal cord and brain.
Side Effect #2: Nausea
Nausea is an uncomfortable and unpleasant sensation where there is an involuntary urge to vomit. Although it is not painful, it can be a debilitating issue as it places discomfort in the back of the throat, chest, and upper abdomen. Like pain, nausea is nature’s way of discouraging the individual from repeating harmful triggers such as ingesting poisonous plants.
It is a common and nonspecific symptom that has various causes such as migraine, dizziness, motion sickness, food poisoning, low blood sugar, gastroenteritis, and increased intracranial pressure. Nausea can be managed using antiemetics such as promethazine, metoclopramide, and ondansetron.
Side Effect #3: Paresthesia
Paresthesia refers to the abnormal sensation in the skin despite no apparent physical cause. This sensation has been reported by patients to be a burning, tingling, prickling, or numbing sensation. The most common kind of paresthesia is often described as pins and needles or the sensation where a limb falls asleep. Paresthesia can be temporary or chronic. Generally painless, it usually occurs in the extremities.
There are many causes of paresthesia such as being in an awkward posture for a prolonged duration, reactive hyperemia, shingles, hypothyroidism, and diseases that cause nerve irritation. In a spinal tap, temporary paresthesia is a side effect, which often affects the lower back and legs.
Side Effect #4: Bleeding into the Spinal Canal
Bleeding into the spinal canal is rare. It can be categorized based on the etiology (nontraumatic or traumatic) or the compartment into which the bleeding occurs (intramedullary, subarachnoid, subdural, epidural). It is most commonly caused by trauma, bleeding diatheses, or vascular malformations. It usually presents as a sudden and painful myelopathy.
While rare, a spinal tap can cause bleeding that results in a spinal hematoma. This usually only occurs if there is preexisting coagulopathy. In these cases, neurosurgical intervention may be beneficial if it leads to further complications such as cauda equina syndrome.
Side Effect #5: Adhesive Arachnoiditis
Arachnoiditis is a condition where the arachnoid mater is inflamed. The arachnoid mater is one of the membranes that surround and protect the brain and spinal cord. Inflammation can occur due to a bacterial infection, viral infection, side effect of chemicals, complications from spinal surgery, chronic compression of spinal nerves, and invasive spinal procedures.
When inflammation occurs, it can result in the formation of scar tissue and adhesion causing the spinal meninges to “stick” together. This is known as adhesive arachnoiditis, an extremely painful condition. Adhesive arachnoiditis is a very rare side effect or complication of a spinal tap.
Side Effect #6: Spinal Cord or Spinal Nerve Trauma
Spinal cord or spinal nerve trauma from a spinal tap will rarely occur. However, accidental puncture can cause severe pain and reflex movement in patients who are conscious.
The needle is inserted between the third and fourth vertebrae or fourth and fifth vertebrae, which is too low to pierce the spinal cord. In most cases, the injury is mild and temporary. Most individuals experience pins and needles on the skin. Other associated symptoms include pain and weakness.
Side Effect #7: Cerebral Herniation
Cerebral herniation or brain herniation is a life-threatening condition where there is very high intracranial pressure causing part of the brain to be squeezed and/or shift past midline. Herniation can occur in intracranial hemorrhage, traumatic brain injury, or brain tumor. When mass lesions such as hematomas occur, cerebral herniation may also occur. Since herniation places pressure on the brain, it can cause blood supply to the brain to be cut off, resulting in tissue death.
Individuals who have cerebral herniation may present with symptoms such as abnormal posturing, vomiting, lowered level of consciousness, and dilation with failed constriction of one or both pupils. In a spinal tap, cerebral herniation can occur if there is elevated intracranial pressure.
Side Effect #8: Back Pain or Discomfort
Back pain can be divided into lower back pain, middle back pain, cervical pain (neck), and coccydynia (tailbone pain). The lumbar area is the most common area affected by pain. Pain can be acute, subacute, or chronic. The character of the pain can be piercing, shooting, or dull. The pain can also radiate into the legs or feet. Other associated symptoms include weakness and paresthesia.
Most back pain occurs due to trauma or degenerative changes to the facet joints or intervertebral discs. Other causes are damaged nerves, muscles, tumors of the vertebra, diseases of the gallbladder, kidneys, aorta, or pancreas. After a spinal tap, there can be back pain in the lower back and legs.
Side Effect #9: Infection
An infection occurs when the host tissues are invaded by disease-causing agents. Infections can be caused by viruses, parasites, and bacteria. The infected host can fight off the infections through their immune system.
Medications used in the treatment of an infection include antibiotics, antivirals, and anthelmintics, and antifungals. In a spinal tap or any other procedure that causes the skin to break, there is a risk of infection. Patients should observe the puncture site for any swelling, redness, warmth, and pain, which may indicate infection.
Side Effect #10: Epidermoid Cyst
An epidermoid cyst is a benign cyst originating from ectodermal tissue. While some patients may not experience any symptoms, others may feel pain and tenderness in the affected region.
Although rare, there are some cases where a spinal tap causes the implantation of epidermoid tissues into the spinal canal during the procedure, which may result in the development of an epidermoid cyst. The risk of an epidermoid cyst is higher when the procedure is performed using a needle without a stylet. Currently, this is an extremely rare occurrence as most spinal tap kits available today contain needles with stylets.