10 Endometriosis Symptoms
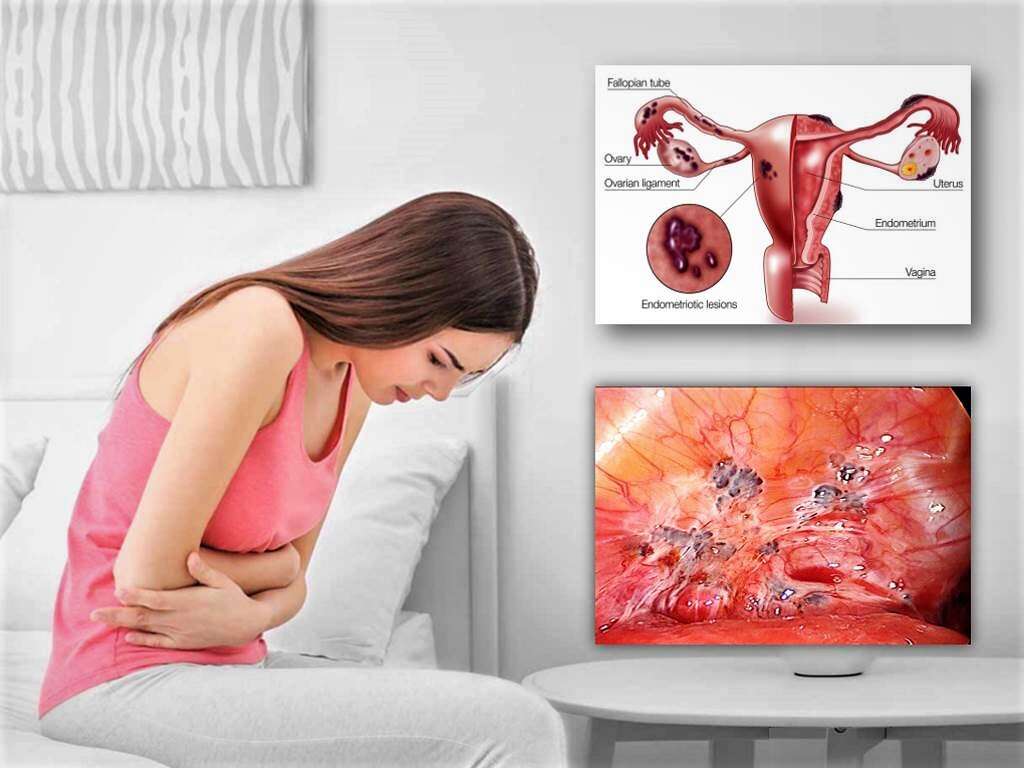
Endometriosis is a chronic condition where the layer of tissue that covers the inner side of the uterus, the endometrium, is found on other sites of the body besides the uterus. This tissue is often found on the fallopian tubes, ovaries, and tissues surrounding them. In rare cases, it can also be found in further parts of the body.
While the cause of endometriosis is not clear, some of the risk factors for endometriosis include having a family history (increased by 7 to 10 times), increased exposure to menstruation (early start of menstruation, heavy bleeding during menses, having short menstrual cycles, or increased duration of menses), conditions that interfere with normal menstrual flow (i.e. fibroids, polyps, structural abnormalities of the uterus), immunologic disorders, and a history of abdominal surgery. Since the affected sites proliferate and bleed (much like intrauterine endometrium) according to the menstrual cycle, they can cause inflammation and fibrosis or adhesions in the surrounding areas. These processes are responsible for the clinical consequences of the condition.
The diagnosis of endometriosis is usually achieved based on symptoms, medical imaging, and biopsy. While there is no cure, management of endometriosis includes pain medication, hormonal treatments, and surgery. It is estimated that approximately 10.8 million women were affected worldwide as of 2015.
Symptom #1: Dysmenorrhea
Dysmenorrhea is a medical term that refers to pain during menstruation or menstrual cramps. It usually starts around the time when menstruation begins and usually lasts no longer than three days. The pain is located in the lower abdomen and may also include back pain (lumbago), nausea and diarrhea. There are two types of dysmenorrhea. Primary dysmenorrhea is menstrual pain without an underlying condition, while secondary dysmenorrhea refers to menstrual pain associated with an underlying disease. Endometriosis is one of the main causes of secondary dysmenorrhea.
Unlike primary dysmenorrhea, secondary dysmenorrhea is more common among women older than 30 years, and gradually worsens with aging. Secondary dysmenorrhea is usually associated with endometriosis, adenomyosis, and uterine fibroids. The mechanism of pain in endometriosis is associated with primary endometriotic lesions (i.e. lesions of the peritoneum that induce inflammatory reactions or ruptured cysts) or secondary lesions (i.e. scar, fibrosis and adhesions may reduce mobility of organs and cause pain).
Symptom #2: Dyspareunia
Dyspareunia is a medical term that is used to describe painful sexual intercourse because of psychological or medical reasons. For some patients, the pain is on the external genitalia while for others, it is felt in the deeper parts of the pelvis. Some studies suggest that women with endometriosis experience higher prevalence of deep dyspareunia than controls.
Women with dyspareunia tend to avoid engaging in sexual activity or can cease it altogether. This can also have an important effect on their self-esteem and relationships. Treatment depends on the underlying cause. In order to reduce the psychosexual sequelae of endometriosis, adequate treatment for the disease should include counselling.

Symptom #3: Dysuria
In medicine, dysuria is a term that refers to pain during urination. It may also be used to describe discomfort or difficult urination. Patients often describe a stinging or burning sensation, that can be caused by many conditions such as endometriosis, urinary tract infection, sexually transmitted diseases, bladder tumors, bladder stones, or medication.
Dysuria most commonly occurs during menstruation in patients with endometriosis.
Symptom #4: Chronic Pelvic Pain
Endometriosis is an important cause of chronic pelvic pain. Among women who undergo laparoscopic surgery for chronic pelvic pain, endometriosis is found to be the cause in a third of cases. Chronic pelvic pain can be debilitating and can lead to recurrent visits to the emergency department, higher likelihood of absence from work, and significant social and physical debility.
Management of chronic pelvic pain includes pain medication, hormonal therapies, and surgery.

Symptom #5: Infertility
Women with endometriosis have a high risk of subfertility of up to 30 to 40 percent. One of the theories on how endometriosis is associated with infertility includes anatomical adhesions around the fallopian tubes or the ovaries that can interfere with the transport of ovarian eggs.
Moreover, endometriosis located in the peritoneum can also interfere with the motility of the fallopian tubes. Infertility in moderate to severe endometriosis can be managed through surgery. Options for achieving pregnancy include and intrauterine insemination, in vitro fertilization and superovulation.
Symptom #6: Fatigue
It is well known that fatigue is one of the most intense and frequent symptoms of this condition. Fatigue among patients with endometriosis is often described as a feeling of constant exhaustion, as if being “tranquilized”. Patients also describe that they are unable to complete their daily activities. Although the mechanism for fatigue in endometriosis is not completely understood, chronic pain plays an important role in its etiology.
Also, the inflammation seen as a response to lesions and the activation of the immune system might be involved in fatigue. Sadly, this symptom is often neglected and frequently goes unnoticed. In the treatment of endometriosis, addressing fatigue, in addition to chronic pain and infertility, is essential to improve the quality of life of these patients.

Symptom #7: Mood disorders
Since endometriosis can cause debilitating symptoms such as pain (i.e. chronic pelvic pain, dysmenorrhea, dysuria), and fatigue, it can significantly compromise social relationships, sexuality, reproduction and mental health. Patients with endometriosis report high levels of depression, anxiety and other psychiatric disorders.
Therefore, psychological assessment is recommended for women with endometriosis, in order to identify patients at risk for developing these symptoms and provide them with adequate psychological support.
Symptom #8: Bowel Symptoms
Bowel symptoms in endometriosis are often overlooked. These are common among women with endometriosis and as many as 60% of afflicted patients have at least one symptom involving the intestinal tract.
Some of the symptoms involving the bowel include painful bowel movements, diarrhea, constipation, abdominal pain, rectal pain, and lower gastrointestinal bleeding (hematochezia).
Symptom #9: Nausea and Vomiting
Nausea and vomiting are observed among patients with endometriosis. Nausea can be defined as a sensation of discomfort and unease in the stomach along with an involuntary urge to vomit. Nausea often precedes vomiting. Vomiting is the forceful expulsion of stomach contents through the mouth and in some cases, the nose.
Both nausea and vomiting are non-specific symptoms and can be seen in many other conditions. Management includes using antiemetics that helps to suppress nausea and vomiting. Patients should try to stay hydrated throughout.
Symptom #10: Headaches and Migraines
Studies show that the prevalence of migraine is significantly higher in patients with endometriosis. The relationship between these conditions is not well understood. Some observations indicate that increased pain sensitivity induced by one of the conditions could make a diagnosis of the other more likely.
This relationship has also been seen in patients who experience fibromyalgia, pelvic pain, irritable bowel syndrome, and interstitial cystitis, where higher rates of migraine have also been observed.